We often speak of a mind-body connection, as though under the right conditions, the mind can talk to the body, and the body can talk back. (This calls to mind the old-fashioned screech of a dial-up modem connection as we try to go online.)
But the breaking story in well-being concerns the relationship between the mind and body (and in addition, the brain). One of the most significant relationships we’ll ever have, it determines our physical, emotional, and social well-being.
For over a decade, I’ve taught what I call the Mind, Brain, and Body Network. If you’ve studied with me in person or online, you’ll notice that the elements have changed over time as emerging research highlights new areas of study. Here’s an up-to-the-moment picture of how I conceptualize this extraordinary communications network and why it holds the key to well-being.
The Mind, Brain, and Body Network.
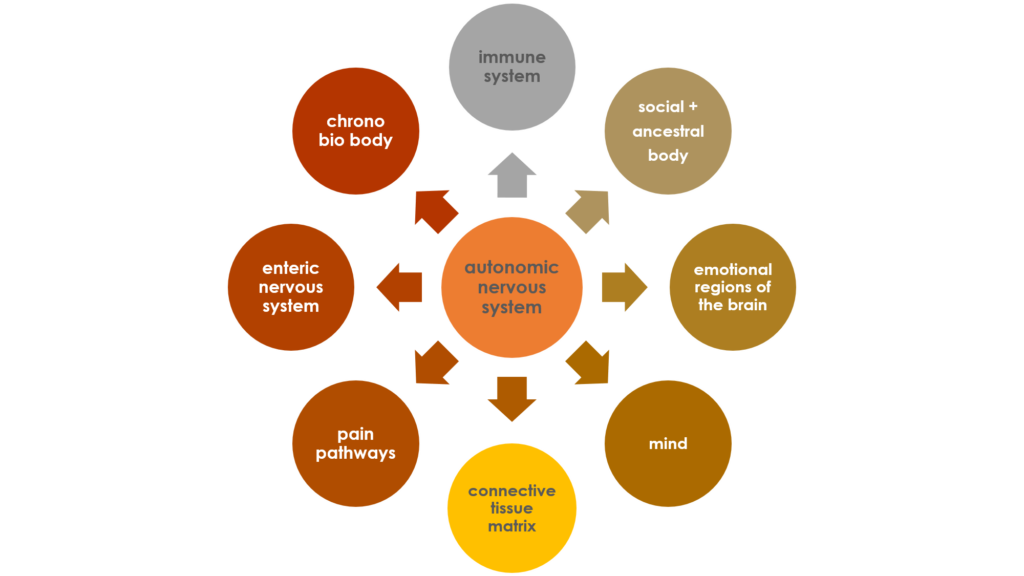
The Autonomic Nervous System acts as the nexus of the mind-brain-body network and our primary regulator of safety. If it slides into hyper-alert mode, you’ll sense a kind of humming or buzzing under the surface. The autonomic nervous system (ANS) regulates functions like heart rate, digestion, rate of respiration, and body temperature. In anxiety, depression, and chronic pain, it can be hyper-activated. And when that happens, the enteric nervous system (or belly brain) and immune system are typically activated at the same time (more on that in a moment).
The Enteric Nervous System (ENS) is currently considered part of the ANS. (I’ve got my doubts about that, and feel intuitively that we might come to believe it’s the other way around.) Housed in sheaths of tissue in the stomach, esophagus, small intestine, and colon, the ENS includes our gut microbiome. A highly intelligent system, it can act independently of direction from the brain and spinal cord. It makes up 75% of our immune system, and is highly linked to mood. One small example: Anxiety makes the stomach more acidic. This upsets the Ph balance of our gut microbiome and makes us likely to have digestive issues like Irritable Bowel Syndrome. And inflammation in our gut disturbs our mood.
Consider the Immune System our primary boundary setter. Its job is to determine what is us and what is not us. (This is why highly empathic people often struggle with boundaries and therefore with autonomic nervous system issues, gut disorders, and chronic inflammation.) The immune system has an extraordinary memory: It can recall the genetic code of any pathogen it encounters (as well as the code that vanquishes it). It can be hyper-active (think auto-immune issues) and respond to everything as a foreign invader. It can be hypo-active and not initiate an alarm response when necessary.
The Mind or Mental Body is the part of us that thinks and reasons. It contains conscious and unconscious thoughts. Like the autonomic nervous system, the mind can be hyper- or hypo-active. In anxiety, for example, thoughts flow rapidly, are hard to anchor, and tend to focus on the future. The mind’s embellishments of our direct experience in the moment and in our body are a cause of our suffering. We often use the terms “mind” and “brain” interchangeably, but consider the brain the neural underpinnings of mental activity.
Our Pain Modulation Pathways regulate the experience we have with pain (and often, with inflammation). These pathways are closely-linked to the ANS, immune system, and mental body (and more). They can be hyper-active and respond to ordinary stimuli as painful. They can also be underactive.
The Emotional Regions of the Brain (Emotional Body) include the limbic system (hypothalamus, amygdala, and hippocampus) but also extend beyond it. Our emotions begin as sensations and thus are linked to interoception, our capacity to sense what’s happening in our body. These regions are tied to our autonomic and enteric nervous systems and our immune system.
The Connective Tissue Matrix is a web of fascia that links every cell in our bodies. It is deeply connected with many elements of the mind-brain-body network, including the autonomic nervous system, enteric nervous system, immune system, pain modulation pathways, and emotional body. Highly sensitive, it has ten times more nerve endings than muscle. Our connective tissue matrix is sentient and intelligent, and plays a role in our sense of cohesiveness.
The Chrono Bio Body has roots in the cyclical and biological rhythms of the body and their relationship with time itself. We have three primary rhythm cycles: Circadian (24 hours), Infradian (longer than 24 hours), and Ultradian (less than 24 hours). These rhythms influence sleep, mood, and well-being. Some rhythms ground our basic rest and activity cycles. (This reinforces the importance of a dynamic rest practices to complement our active ones.)
Think of our Social Body, made up of relationships, as the social connective tissue that binds us and makes us responsible to one another. These relations (including ancestors who came before us, descendants, our kinship with land and climate and all living things) knit us together and shape our collective. Like the immune system, the social body has boundaries which can be hyper-active and respond to ideas, experiences, and people as though they are “not us.” Most modern yoga and mindfulness settings overlook the social body, and this is to our detriment as a collective.
_____________________________
The mind, brain, and body are a system.
Each element (body) extends its filaments deep into the others. The bodies are interdependent. In fact, if the diagram above were technically accurate, you’d see arrows in each direction and between every body in the network. (In that case, the diagram would be a mess, so forgive me for taking liberties to make it clearer and easier to view.)
Looking at this network as a dynamic, interactive, intelligent system expands our vision about what anxiety (or depression or chronic pain or inflammation or any other mind-body dis-ease) really is. This vision offers avenues for intervention, for building physical, emotional, and collective well-being.
So what is a “mental health issue,” exactly, and how can we balance it?
Anxiety, depression, chronic pain, and inflammation are not just “mental” or “emotional” problems but patterns expressed and practiced by the entire mind-brain-body network.
Each body “practices” its own version that contributes to the larger mosaic of anxiety, depression, or chronic pain.
Here’s what that looks like in real time. In anxiety, for example, the autonomic nervous system “practices” hyper-arousal. The immune system “practices” an inflammatory response- its own version of ANS hyper-arousal. The connective tissue matrix “practices” tension and dehydration. The mind practices worried, catastrophic, future-focused thinking. All this happens simultaneously, and strengthens the pattern of anxiety across the mind, brain, and body network.
Depression works in much the same way, as do chronic pain, addictions, and many more emotionally-mediated illnesses.
The good news is that each body in the mind, brain, and body network can learn a different way of practicing.
To build emotional balance, we need to address the pattern not just in one or two or three elements, but throughout the entire Network. We can teach each element to practice something other than anxiety–in other words, to practice not-anxiety.
One of the biggest disservices we do as medical doctors, psychologists, yoga teachers, or proponents of other mind-body practices is to give people the impression that medication and psychotherapy are all we need. Or that yoga or mindfulness determine our emotional health.
Two decades of data gathering in mental health and mind-body research have taught us that psychotherapy, medication, yoga, or mindfulness alone (or in combination) don’t improve anxiety and depression enough. Psychotherapy addresses the mind, emotional body. and sometimes the social body. Medication affects the nervous system and emotional regions of the brain. Mindfulness and yoga therapy address the mind, pain pathways, emotional regions of the brain, and sometimes the nervous system or immune system.
The end result: addressing the mind and emotions (through psychotherapy) and the emotional regions of the brain and the autonomic nervous system (through, say, medication). Yet in the meantime, the other bodies continue to practice anxiety or depression, and the pattern remains strong.
It’s important that we use all the arrows in our quiver (yoga, mindfulness, psychotherapy, medication, embodiment, exercise, lifestyle changes, and much more) to balance anxiety and build resilience. Yet where do we start?
To focus our therapeutic plan, it helps to target the “first responders” in anxiety, depression, or chronic pain.
These are the elements of the mind-brain-body network that practice specific emotional patterns most powerfully and are “easiest” to access. When it comes to depression, for example, the first responders are:
- the autonomic nervous system
- enteric nervous system
- immune system
- mind
- social body
(The same is true for seasonal affective disorder, which shares several first responders with depression).
This perspective can fundamentally changes the way we practice, teach, and live. It makes our efforts more integrated and therapeutic. My philosophy embraces a mind-brain-body approach to emotional health which includes psychotherapy, meditation, yoga, and medication, but doesn’t stop there.
Very helpful explanation because it was clearly explained in the circular diagram plus the descriptions in the blog.
Such an elegant approach that sees the beauty of being human as a dynamic and interactive model of relationship that makes up a functional system. Your work and the exquisite way you present it is so needed, thank you!
Thank You for your information.